Shin Splints
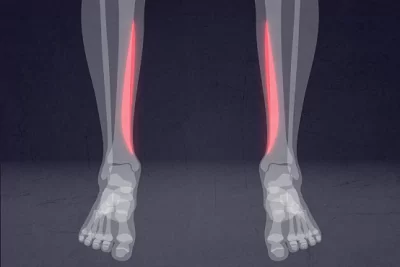
Shin Splints (Medial Tibial Stress Syndrome) is a condition characterised by damage and inflammation of the connective tissue joining muscles to the inner shin bone (tibia).
There are several muscles which lie at the back of your lower leg and are collectively known as the calf muscles. Several of these muscles lie deep within the calf (tibialis posterior, flexor digitorum longus, flexor hallicus longus and soleus) and attach to the inner border of the shin bone (tibia). The connective tissue responsible for attaching these muscles to the tibia is known as the tenoperiosteum. Every time the calf contracts, it pulls on the tenoperiosteum. When this tension is too forceful or repetitive, damage to the tenoperiosteum occurs. This results in inflammation and pain and is known as medial tibial stress syndrome– commonly referred to as shin splints.
Medial tibial stress syndrome can sometimes occur in combination with other pathologies that cause shin pain such as compartment syndrome and tibial stress fractures.
N.B. Medial tibial stress syndrome has only recently fallen into the catergory of shin splints, the main conditions that fall into this catergory are; stress fracture, myositis, periositis, tendinotis, compartment syndrome, fasciitis and ischaemic disorders.
Causes of shin splints
Shin splints most commonly occur due to repetitive or prolonged activities placing strain on the tenoperiosteum. This typically occurs due to excessive walking, running or jumping activities (such as an increase in physical exercise) and is often seen in runners and footballers. It frequently occurs in combination with calf muscle tightness or other biomechanical abnormalities, such as excessive pronation or supination (high arch), or in those who consistently wear inappropriate footwear. Athletes more commonly develop this condition early in the season following a period of reduced activity (deconditioning) and when training surfaces are generally harder.
Signs and symptoms of shin splints
Patients with shin splints typically experience pain along the inner border of the shin. In less severe cases, patients may only experience an ache or stiffness along the inner aspect of the shin that increases with rest (typically at night or first thing in the morning) following activities which place stress on the tenoperiosteum. These activities typically include excessive walking, running (especially up hills, on uneven surfaces or in poor footwear), jumping and general weight bearing activity.
The pain associated with this condition may also warm up with activity in the initial stages of injury. As the condition progresses, patients may experience symptoms that increase during sport or activity, affecting performance. In severe cases, patients may walk with a limp, although this may also reduce to some extent as the patient warms up.
Patients with this condition typically experience pain on firmly touching the inner border of the shin bone, particularly along the lower third of the bone. Areas of muscle tightness, thickening or lumps may also be felt in the area of pain. In severe cases, swelling, redness and warmth may also be present.
Prognosis of shin splints
Most patients with this condition heal well with appropriate treatment. Recovery time may range from a few weeks to many months depending on the severity of injury, quality of treatment and length of time the injury has been present for. Patients with shin splints that have been present for months may require a considerable period of treatment associated with reduced activity before full recovery occurs.
Contributing factors to the development of shin splints
There are several factors which can predispose patients to developing this condition. These need to be assessed and corrected. Some of these factors include:
- Excessive training or activity
- Poor foot posture
- Inappropriate footwear
- Inadequate warm-up
- Training on hard or inappropriate surfaces
- Muscle weakness (especially the calf muscles)
- Tightness in specific joints (such as the ankle)
- Tightness in specific muscles (especially the calfs)
- Poor lower limb biomechanics
Shin Splints Treatment
It is important to highlight that the best treatment for shin splints is treating the cause, rather than the symptoms, as previously discussed there has been a lot of research conducted which shows a rolled in foot/ over pronated foot or high arch foot will cause shin splints. By changing and optimizing foot and leg biomehcanics, we can treat the condition of shin splints. There are ways of dealing with the pain in-between time which include;
- Deep tissue massage (particularly to the calf muscles)
- Joint mobilization
- Taping
- Orthotics
- Biomechanical correction
- Progressive exercises to improve flexibility (especially of the calf muscles)
- Activity modification advice
- Footwear advice
How Can We Help?
Follow the form below to get through directly to one of our Podiatrists at the practice or to request an appointment.
Or call — 01444 453874
"*" indicates required fields
